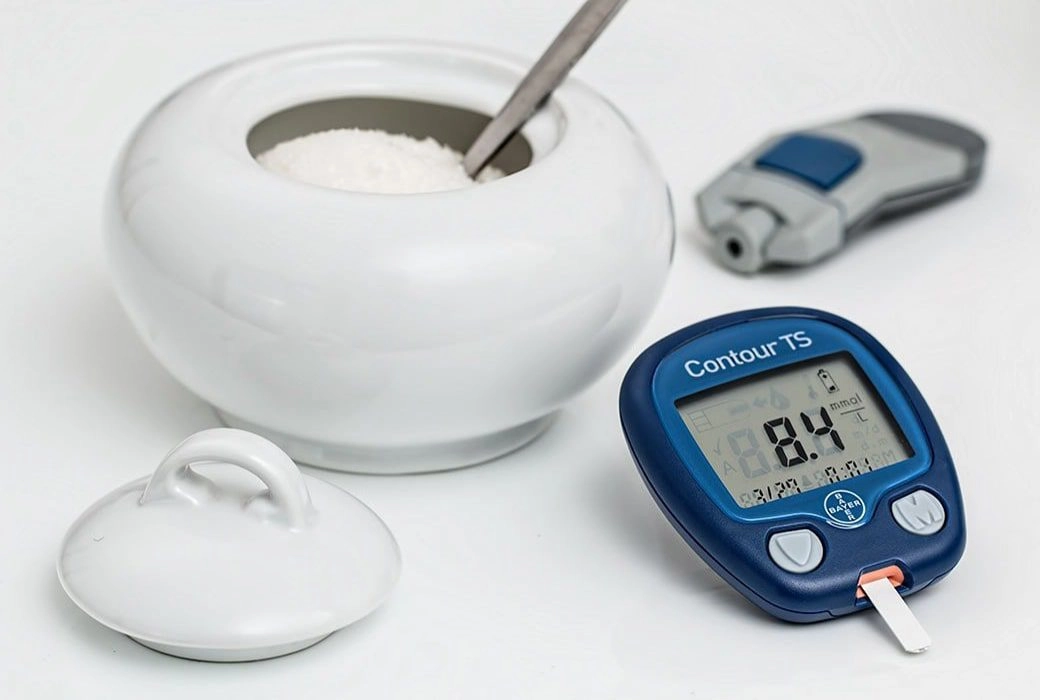
Diabetes is a disease that results from the body losing the ability to maintain healthy blood sugar levels. Regulating the levels of sugar, or glucose, in the bloodstream is normally the job of the pancreas, a gland that is located below and behind the stomach. In most people, as your Anchorage chiropractor can explain, the pancreas produces insulin, which allows sugar from food to enter cells and helps control the level of glucose in the bloodstream.
In diabetic individuals, the pancreas produces little or no insulin. As a result, blood sugar levels must be adjusted through other means. This typically includes careful diet and exercise, medication, insulin therapy, or a combination of these techniques. Someone with diabetes is at risk of hyperglycemia (abnormally high blood sugar levels) and hypoglycemia (abnormally low blood sugar levels), and the many health risks that are associated with these conditions.
There are two distinct forms of the disease: Type 1 and Type 2. Type 1 diabetes accounts for less than 10% of all diabetes diagnoses in the United States. According to the American Diabetes Association, this less common form of the disease still affects up to 1.25 million Americans.
This type of diabetes poses a lifelong risk of complications and demands constant monitoring of blood sugar levels and food intake. Mary Tyler Moore, who served as an International Chairman for the JDRF (formerly the Juvenile Diabetes Research Foundation), described her experience with the disease like this:
“Both children and adults like me who live with Type 1 diabetes need to be mathematicians, physicians, personal trainers, and dietitians all rolled into one. We need to be constantly factoring and adjusting, making frequent finger sticks to check blood sugars, and giving ourselves multiple daily insulin injections just to stay alive.”
Although Type 1 diabetes is a frightening condition, learning about the causes, symptoms, and treatment options is the most important way to take charge of your own health.
Top Anchorage Chiropractor: What Is Type 1 Diabetes?
Type 1 diabetes is sometimes known as juvenile diabetes. This moniker has been applied to Type 1 because it frequently develops in children and adolescents under 20 years of age. The disease is most commonly diagnosed either between the ages of four and seven, or between the ages of 10 and 14.
However, the term “juvenile diabetes” is misleading in a number of ways. For one thing, Type 1 diabetes can appear at any age. Every year, roughly 15,000 children are diagnosed with the disease. The number for adult diagnoses is nearly identical — about 15,000 a year.
Additionally, a child that is diagnosed with diabetes doesn’t necessarily have Type 1. It’s becoming more and more common for children to suffer from Type 2 diabetes.
While Type 1 diabetes is typically a combination of an autoimmune issue and a genetic predisposition, Type 2 diabetes is often considered a lifestyle disease. The most common risk factors for Type 2 diabetes are obesity and lack of physical activity. As childhood obesity becomes more prevalent, Type 2 diabetes also becomes more common in children and adolescents.
What Are the Causes of Type 1 Diabetes?
Hereditary Causes
The main risk factors for Type 2 diabetes are diet and exercise. Almost anyone can develop Type 2 based on these two factors (although numerous other factors, such as age, ethnic background, genes, and family history also play a role).
However, current evidence suggests that only certain people have a genetic predisposition to Type 1 diabetes. Scientists have discovered that only people with a specific human leukocyte antigen (HLA) complex can develop the disease.
Different HLA complexes affect the way the body responds to infection. These complexes are responsible for triggering an autoimmune response when the body encounters a virus. A number of specific HLA complexes have been associated with the development of Type 1 diabetes. All of the Type 1-correlated HLA complexes are located on chromosome 6.
Type 1 diabetes isn’t the only autoimmune disease associated with the presence or absence of certain HLA complexes. Other HLA complexes have been identified that correlate to diseases such as rheumatoid arthritis, juvenile rheumatoid arthritis, or ankylosing spondylitis.
Autoimmune Triggers
Simply having an HLA complex that’s associated with Type 1 diabetes isn’t enough to develop the disease. Something needs to trigger one of these HLA complexes to begin producing antibodies. Most commonly, the trigger is a viral infection.
When a virus enters the body, it sets off a reaction in the immune system. T cells are a key part of the immune system’s defenses. These T cells begin producing antibodies that attack the virus cells. The T cells themselves also assist in fighting off the infection.
Beta cells are one of the cell types that make up islets of Langerhans, which are clusters of cells in the pancreas responsible for insulin production. Certain viruses have antigens that are very similar to the antigens of beta cells. Diseases that are theorized to have antigens similar to those of beta cells include:
- Rubella (although so far only congenital rubella has been definitively associated with Type 1 diabetes)
- Mumps
- Coxsackie B4 Virus (sometimes known as CVB4)
- Rotavirus
When someone has an HLA complex that predisposes them to Type 1, contracting one of these viruses can cause the onset of diabetes.
The T cells will recognize the virus and launch an autoimmune attack on the virus cells. However, the T cells might confuse the antigens of the virus with the antigens of the body’s own beta cells. If the T cells begin to attack the beta cells in the pancreas, they can eventually kill off all of the beta cells.
This isn’t an immediate process. It may take years for the T cells to destroy most or all of the beta cells. Once the majority of the insulin-producing beta cells have been destroyed, the body is no longer able to regulate the glucose levels in the blood. Type 1 diabetes is the result.
There may also be a correlation between Type 1 diabetes and numerous strains of enterovirus. Scientists have found that enterovirus antibodies are detected at elevated levels in pregnant women whose children will eventually develop Type 1 diabetes. Children who contract an enterovirus infection after birth are more likely to develop Type 1 diabetes than their siblings who do not contract an enterovirus.
Other Causes
Although there has been extensive research into Type 1 diabetes, doctors aren’t entirely certain what factors might cause the disease. Besides an autoimmune response to a viral infection gone wrong, various other theories have been proposed to account for the development of the disease.
Some experts suggest that Vitamin D might play a role in Type 1 diabetes. The overall incidence of the disease tends to increase in populations farther away from the equator — so someone living in the far northern or far southern hemisphere is more likely to develop Type 1 diabetes than someone living near the equator. Canada, the United Kingdom, Australia, and numerous Scandinavian countries have all been found to have a higher incidence of Type 1 diabetes when compared to the worldwide average.
This could suggest that sun exposure and the Vitamin D it supplies might have an effect on pancreas function and insulin production. Additionally, there is evidence that regularly taking Vitamin D supplements is correlated to a lower risk of Type 1 diabetes.
A number of studies have suggested that drinking cow’s milk as an infant may also impact the risk of Type 1 diabetes. According to this research, the infant’s body might mistake the protein in the cow’s milk as a foreign invader. When the baby’s immune system attacks those proteins, it may also attack a naturally occurring protein called glycodelin.
This protein helps regulate T cell production. When the immune system attacks the glycodelin proteins, it can lead to an overproduction of T cells. These T cells, in turn, can attack the beta cells in the pancreas. It’s important to note, however, that these studies are controversial. A link between introducing cow’s milk to infants and a heightened risk of Type 1 diabetes has not been conclusively established.
In very rare cases, diabetes might be the result of external damage to the pancreas. Physical trauma that causes damage to internal organs might affect the ability of the pancreas to create insulin. Certain types of toxins might also interfere with insulin-producing functions. Other medical conditions that necessitate the partial or total removal of the pancreas could also lead to the onset of diabetes.
How Can Type 1 Diabetes Be Controlled? – Anchorage Chiropractor Answers
For individuals who have diabetes, maintaining good blood sugar is extremely important. Unmanaged diabetes can lead to wide-ranging and potentially life-threatening complications. The main risks for sufferers of diabetes include:
- Nerve damage (neuropathy), particularly in the feet and legs
- Eye problems, such as cataracts, glaucoma, and diabetic retinopathy
- Cardiovascular disease, such as heart attack, stroke, and high blood pressure
- Kidney damage, which may be severe enough to require dialysis or a kidney transplant
Because the consequences of unmanaged diabetes can be so serious, it’s important that diabetics learn all they can about the disease and how to best care for themselves.
Both Type 1 and Type 2 diabetes are related to how the pancreas produces insulin. With Type 2 diabetes, insulin management typically means maintaining a healthy diet, getting plenty of exercise, and monitoring blood sugar levels as necessary. It may also mean medication or insulin therapy, depending on the severity of the condition.
Type 1 diabetes always requires insulin therapy. Insulin is most commonly administered through injections, which diabetics typically learn how to give to themselves. The insulin is injected directly under the skin so that it can act as a replacement for the insulin that the pancreas isn’t able to produce. Doctors have noted some of the best results with a regimen of three or more insulin injections per day, which helps to mimic the body’s natural rhythm of glucose regulation.
Some diabetics choose to use an insulin pump instead of utilizing self-administered injections. A standard insulin pump is about the size of a cell phone, and is worn outside the body. A small reservoir of insulin is attached to a catheter tube that is inserted under the skin, most often on the abdomen. The pump can then be programmed to dispense specific amounts of insulin at designated times, allowing the wearer to maintain a steady blood sugar level throughout the day.
Recently, medical experts have developed wireless insulin pumps. These pumps require small pods containing the insulin to be worn outside the body, while a small catheter allows the insulin to get underneath the skin. A wireless pump can be placed on the abdomen, like a typical insulin pump, or on the lower back, arm, or leg. The pods are connected to a wireless device, which can be used to program the intervals and doses of insulin based on the type of food that the wearer eats.
Many people with diabetes have been able to very effectively control their blood sugar levels with any of these methods. It’s important to note that insulin is not a cure; it’s a lifelong therapy that must be administered on a daily basis. However, with good management, individuals with Type 1 diabetes can live full, active lives just like anyone else.
Living with Type 1 Diabetes
Type 1 diabetes is a complicated condition that doesn’t always have a single, clear-cut cause. Because of the various treatment options available, it might take a while for a newly diagnosed individual to find a method that works for them.
By working closely with medical professionals and a support network of loved ones, individuals with this disease can control their blood sugar levels and avoid many of the health risks associated with diabetes. Even young children who are diagnosed with this illness can learn to manage their condition and keep themselves healthy.
If you need more information about the causes, symptoms, and treatment options for Type 1 diabetes, visit the Mayo Clinic website or the American Diabetes Association website.